 This risk assessment tool is likely to be clinically useful in the triage and management of fibrinolytic-eligible patients with STEMI. The TIMI risk score for STEMI captures the majority of prognostic information offered by a full logistic regression model but is more readily used at the bedside. Calculation of the TIMI Risk Score for STEMI History of diabetes mellitus or hypertension or angina, 1 Systolic blood pressure <100, 3 Heart. External validation in the TIMI 9 trial showed similar prognostic capacity (c statistic 0.746). The prognostic performance of the risk score was stable over multiple time points (1 to 365 days). The prognostic discriminatory capacity of the TIMI risk score was comparable to the full multivariable model (c statistic 0. The risk score showed a >40-fold graded increase in mortality, with scores ranging from 0 to >8 (P:<0.0001) mortality was <1% among patients with a score of 0. Ten baseline variables, accounting for 97% of the predictive capacity of the multivariate model, constituted the TIMI risk score. In the multivariate analysis, weight < 67 Kg, previous infarction, left bundle branch block and hypertension did not show statistical significance. The Thrombolysis in Myocardial Infarction (TIMI) risk score for STEMI was created as the simple arithmetic sum of independent predictors of mortality weighted according to the adjusted odds ratios from logistic regression analysis in the Intravenous nPA for Treatment of Infarcting Myocardium Early II trial (n=14 114). The TIMI risk score for STEMI showed a discriminatory power of 0.82, with no identification of new predictors of mortality. We developed and evaluated a convenient bedside clinical risk score for predicting 30-day mortality at presentation of fibrinolytic-eligible patients with STEMI. Aim: To determine the association between TIMI risk score and in-hospital mortality and adverse events in acute STEMI patients undergoing primary PCI at a. The receiver operating characteristic curve (ROC) of TIMI risk score for in-hospital mortality and short-term mortality are presented in Fig 1. Complex multivariable models identify independent predictors and quantify their relative contribution to mortality risk but are too cumbersome to be readily applied in clinical practice. Based on the Youden Index the optimal cut-off value of TIMI risk score was found to be 6 with sensitivity of 69.2, specificity of 61.6, and overall accuracy of 62.1. These tools include predictors of poor outcomes identified in large databases of patients with STEMI. We prefer the TIMI risk score or the GRACE risk model. 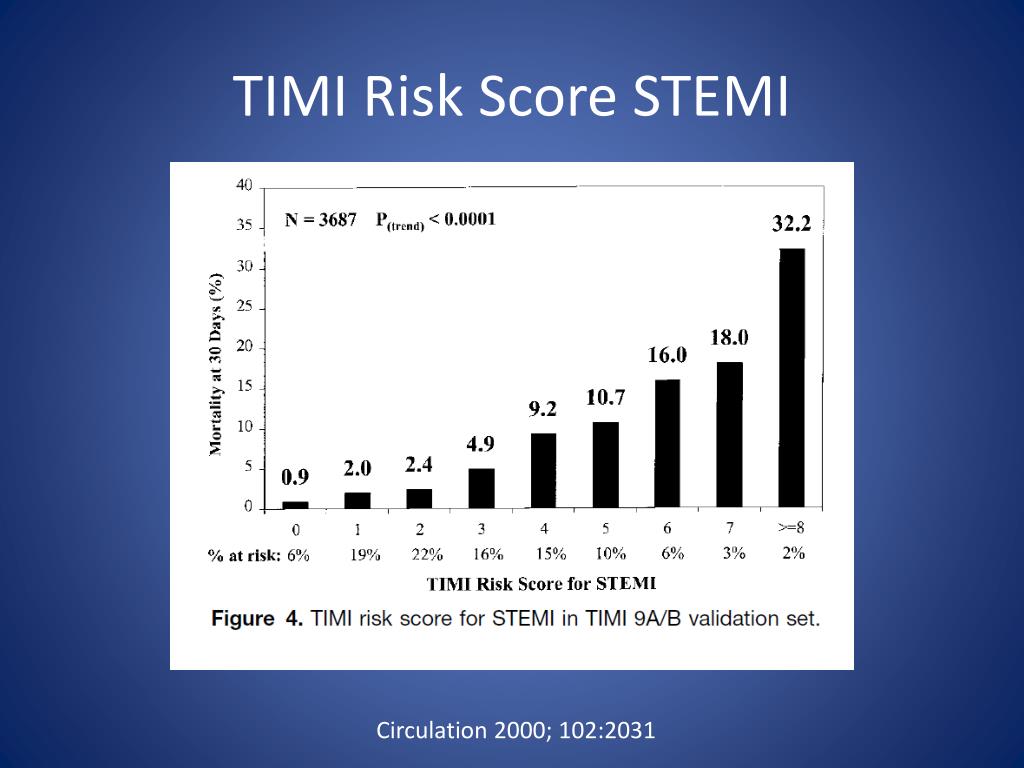
Considerable variability in mortality risk exists among patients with ST-elevation myocardial infarction (STEMI). All STEMI patients should undergo risk assessment with one of the tools presented below within the first four to six hours of hospitalization. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
